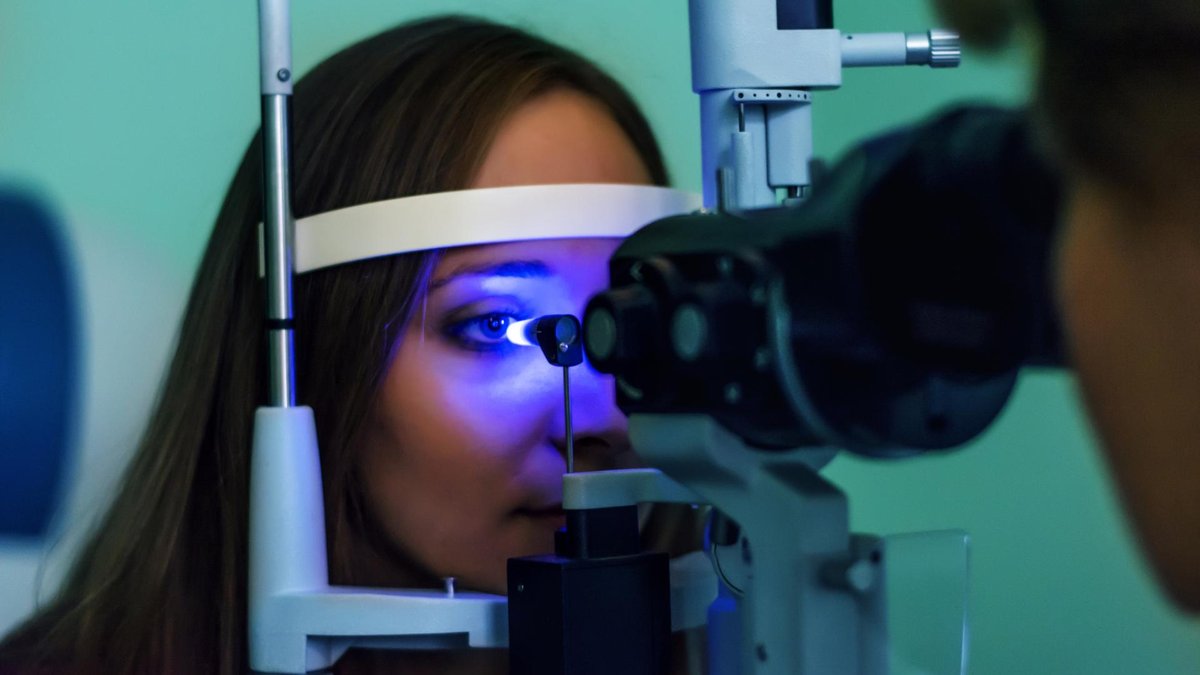
When people hear the word “glaucoma,” many of them connect the eye disease with elevated eye pressure (also known as intraocular pressure or IOP). However, the relationship between glaucoma and eye pressure is complicated and has changed over time.
Historically, glaucoma was identified as a disease in which the eye was firm or hard due to high eye pressure. However, doctors gradually came to understand that glaucoma can occur even when eye pressure is normal, which sometimes makes it harder to diagnose. In addition, patients with high eye pressure sometimes do not experience any pain and do not have any glaucoma symptoms. Today, eye pressure is considered a major risk factor for glaucoma but is not included in the definition of this eye disease. However, eye pressure control continues to play a major role in the treatment of glaucoma. Lowering eye pressure is the only treatment we currently have, whether through medications, laser, or surgery.
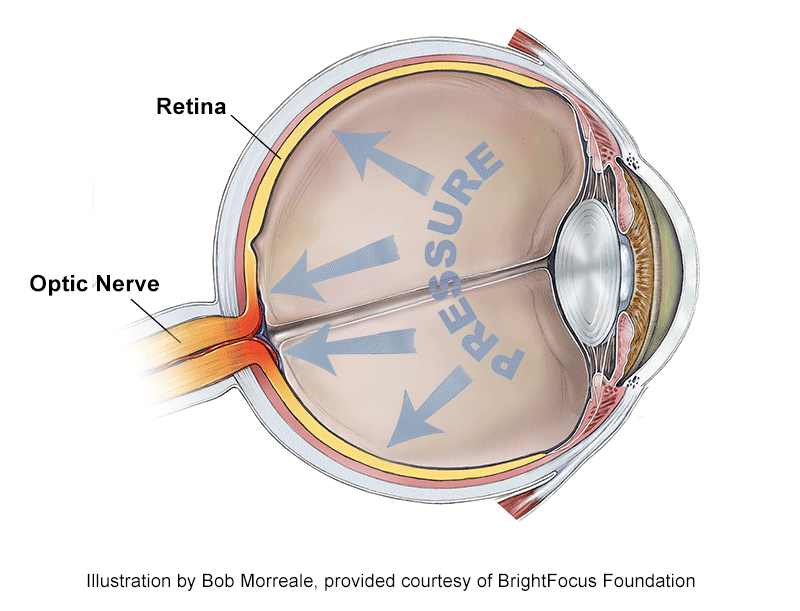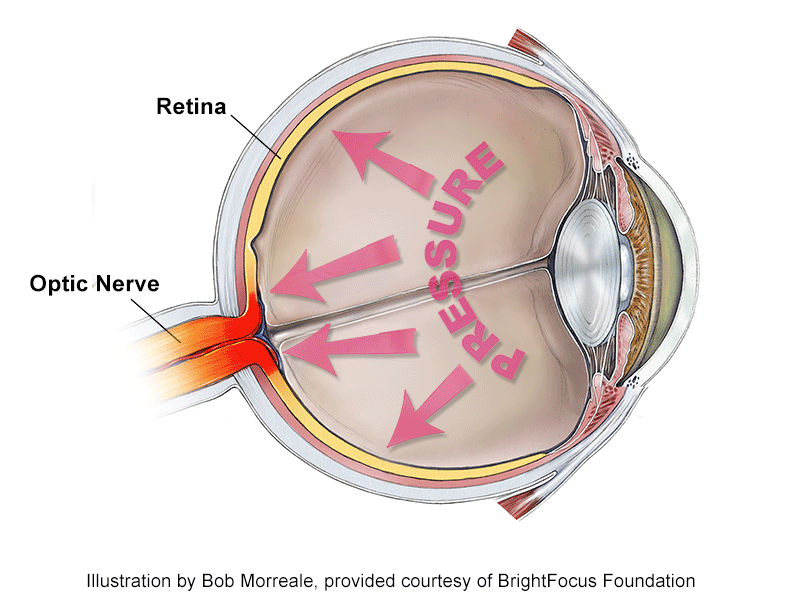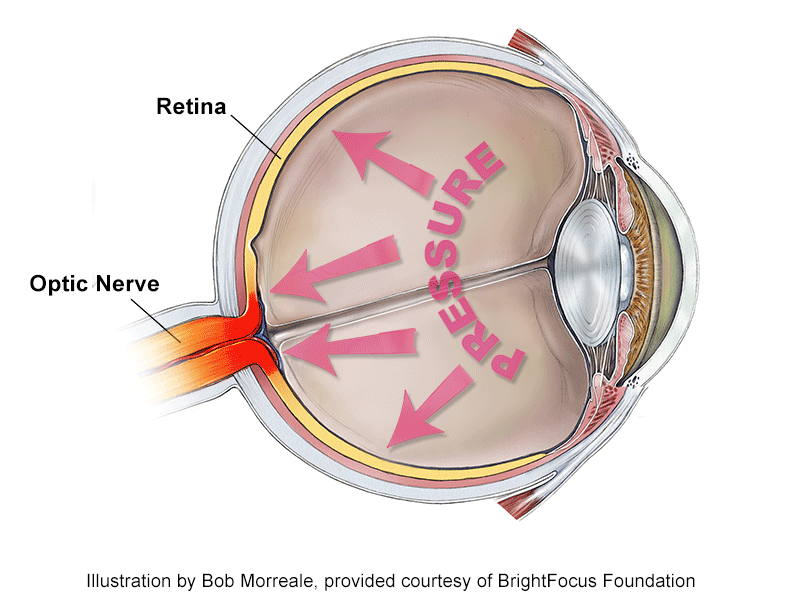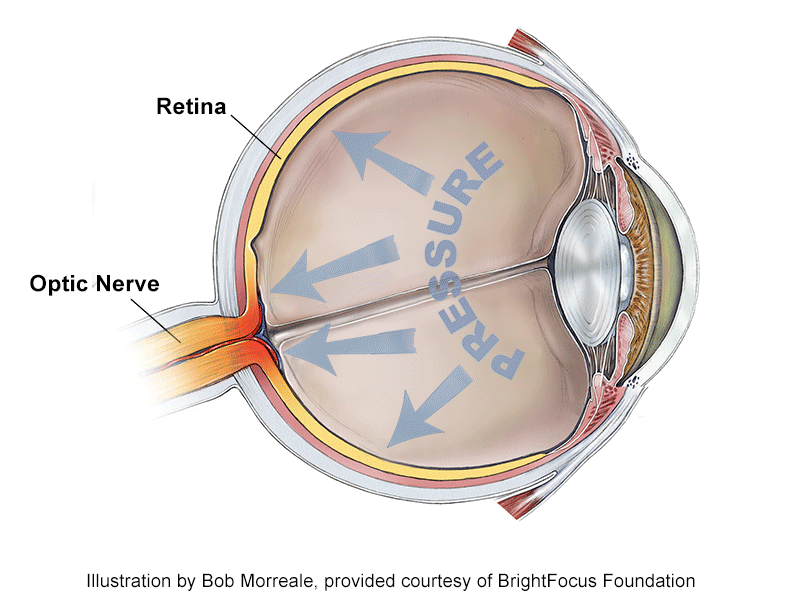
What is Considered High Eye Pressure?
In many forms of glaucoma, the eye pressure is high. What is considered “too high”? Patients ask me this all the time, and I tell them it depends.
First, we know that statistically speaking, having eye pressures over 21 mmHg (millimeters of mercury) is not very common in a generally healthy population. We also know that eye pressure tends to increase as we get older since the drainage system does not function as well.
Second, we know that an optic nerve that is healthy can withstand a higher eye pressure than an optic nerve that is unhealthy. For example, patients who have optic nerves that already have signs of damage likely need lower eye pressures to prevent worsening of glaucoma.
Third, the eye pressure that is “too high” for your optic nerve is sometimes determined over time. Let’s say you begin treatment with an eye drop to lower eye pressure, and it is successful in lowering your eye pressure by 20 percent. However, your glaucoma continues to progress slowly. In that case, despite the initial eye pressure lowering, your ophthalmologist may determine that this new lower eye pressure is still “too high” and your eyes need to have even lower eye pressure.
Finally, it is important to realize that most patients with the most common form of glaucoma, primary open-angle glaucoma, have elevated eye pressures but do not feel pain or have other symptoms. Glaucoma is often called the “silent thief of sight” because patients do not have symptoms until late in the disease when they notice central vision loss.
Glaucoma with “Normal” Eye Pressure
Another form of glaucoma is called normal-tension glaucoma. If someone has normal-tension or normal-pressure glaucoma, their eye pressure has never been recorded above 21 mmHg, yet they still have optic nerve damage. Does this mean that their eye pressure has never been greater than 21 mmHg? That is difficult to say since a single eye pressure measurement at any given time on any given day in the ophthalmologist’s office is a tiny “snapshot” of what the eye pressure truly is. Normal-tension glaucoma is likely not a truly separate disease from primary open-angle glaucoma, but rather the same disease in which other factors such as blood flow to the optic nerve may also play an important role.
Patients who have normal-tension glaucoma are thought to have more susceptible optic nerves, such that even at normal eye pressures the optic nerve slowly degenerates. Moreover, even though the eye pressure is “normal,” the treatment is the same: lowering the eye pressure through medications, laser, or surgery. Lowering eye pressure in normal tension glaucoma patients was found to slow glaucoma progression in well-designed randomized clinical trials including the Collaborative Normal Tension Glaucoma Study (CNTGS). The CNTGS was the first study of its kind to show that a 30 percent decrease in eye pressure reduced disease progression in patients with normal-tension glaucoma.
Aiming for the Target
One term you may hear your ophthalmologist discuss is your “target eye pressure.” This refers to a goal eye pressure your ophthalmologist believes will stop your glaucoma from worsening. There is no magic formula but it is based on the status of your optic nerve, the results of your visual field tests, and your ophthalmologist’s clinical judgment, among other factors. It is a good goal to have, but it is not the only factor to consider. And, even though you may have a target eye pressure, it is important to recognize that a single eye pressure measurement in the office is not truly reflective of what your eye pressure is on average, day to day, week to week, or month to month.
Finally, your target eye pressure may change over time depending on how stable your glaucoma is. For example, if you have been stable for a long time, your ophthalmologist may not be as concerned by an eye pressure measurement that is slightly above goal. Indeed, eye pressure can vary depending on the time of day, when you instilled your last dose of eye drops (if you are on medication), your stress level, and other factors. On the other hand, if you continue to demonstrate worsening glaucoma despite being at your target eye pressure, your ophthalmologist may decide to revise the target pressure to an even lower goal.
About BrightFocus Foundation
BrightFocus Foundation is a premier global nonprofit funder of research to defeat Alzheimer’s, macular degeneration, and glaucoma. Since its inception more than 50 years ago, BrightFocus and its flagship research programs—Alzheimer’s Disease Research, Macular Degeneration Research, and National Glaucoma Research—has awarded more than $330 million in research grants to scientists around the world, catalyzing thousands of scientific breakthroughs, life-enhancing treatments, and diagnostic tools. We also share the latest research findings, expert information, and resources to empower the millions impacted by these devastating diseases. Learn more at brightfocus.org.
Disclaimer: The information provided here is a public service of BrightFocus Foundation and is not intended to constitute medical advice. Please consult your physician for personalized medical, dietary, and/or exercise advice. Any medications or supplements should only be taken under medical supervision. BrightFocus Foundation does not endorse any medical products or therapies.
- Eye Pressure
- Risk Factors









