Geographic Atrophy
Some people with age-related macular degeneration (AMD) will develop geographic atrophy, an advanced and severe form of dry AMD that can lead to permanent vision loss.
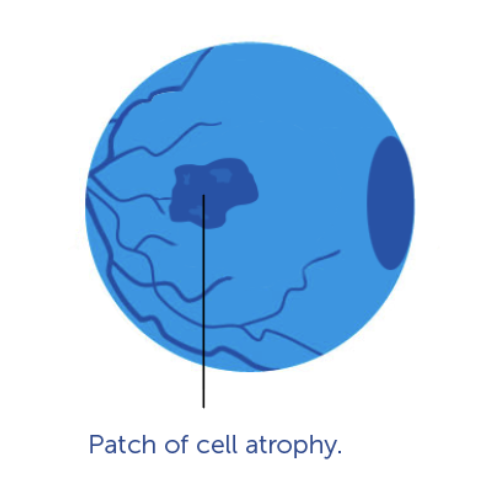
What is Geographic Atrophy?
Geographic atrophy is an advanced and severe form of dry age-related macular degeneration. In geographic atrophy, regions of cells in the retina waste away and die (atrophy). Sometimes these regions of atrophy look like a map to the doctor who is examining the retina, hence the term geographic atrophy. The regions of atrophy result in a blind spot in the visual field. Geographic atrophy can affect one or both eyes, and a patient with the disease in one eye is more likely to develop it in the other.
Geographic atrophy causes around 20% of legal blindness in North America. An estimated five million people worldwide have geographic atrophy, with roughly one million of them living in the United States.
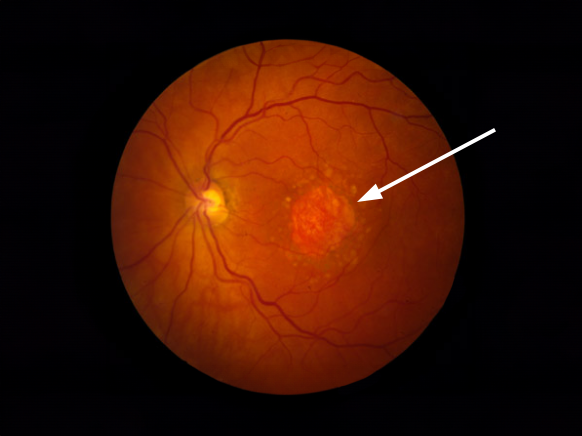
Symptoms of Geographic Atrophy
In early dry macular degeneration, cells in the macula begin to waste away and die (atrophy), and parts of central vision become blurry. This may be difficult to notice at first, especially if the other eye is healthy, which can often hide the problems of the affected eye. Some people may find that they need more light to read but otherwise may not notice problems with their vision.
As dry macular degeneration slowly progresses, the blurring worsens and increases in size. Some permanent blind spots (called scotomas) in the visual field may develop. The person may begin to have trouble telling the difference between similar colors, or shades of the same color.
Symptoms of geographic atrophy include:
- Difficulty reading in dim lighting
- Poor night vision
- Central vision loss, including difficulty seeing faces, cooking, driving, etc.
- Black spot in central vision
- Slower reading speed; one or several letters in a word appear “missing”
- Difficulty distinguishing between different shades
- Trouble with glare
Risk Factors for Geographic Atrophy
Certain risk factors increase a person’s chances of developing dry macular degeneration and geographic atrophy, including:
- Being older than 60
- Having a family history of macular degeneration
- Smoking or having smoked in the past
- Being obese
- Having light-colored eyes
- Spending a lot of time in the sun
- Caucasians are more likely to develop it than African Americans or Hispanics
- Eating a high-fat diet and/or low in nutrients and antioxidants
- Inactivity
Diagnosing Geographic Atrophy
If you have already been diagnosed with dry macular degeneration, ask your doctor how often you need to be monitored for potential progression to geographic atrophy.
A dilated eye exam is the first step to diagnosing geographic atrophy. The following imaging techniques can also be used in diagnosing or monitoring geographic atrophy:
Treatments for Geographic Atrophy
The first treatments for geographic atrophy were approved by the U.S. Food and Drug Administration in 2023. The first, Syfovre, was approved in February 2023, followed by Izervay in September 2023. Both treatments slow the progression of the disease by targeting inflammation in the complement pathway system in the eye.
Macular Degeneration Research, a BrightFocus Foundation program, funds innovative research into new drugs and ways to manage and treat this complex form of AMD.
Living Well With Geographic Atrophy
Despite its severity, macular degeneration usually doesn’t affect both eyes equally. Many people find they can adapt and function by making the most of their remaining vision; some find new ways to accomplish their daily activities through vision rehabilitation. Certified low-vision therapists can help you make the most of your remaining vision with special vision aids and devices such as magnifiers, and occupational therapists can help you do everyday tasks and chores, such as setting up your kitchen, bathroom, lighting, etc., in new ways. These two types of low-vision evaluations are typically reimbursable by private insurers and Medicare.
Your initial visits to these specialists are not just a one-time experience. These doctors will help you adapt as your vision continues to change. With this type of professional assistance, you can learn to develop new ways of doing the things you love as your vision changes and maintain your independence and quality of life.
To preserve remaining vision, it’s important to protect your eye health. Here are a few steps to take:
- If you are a smoker, stop right away.
- Eat a healthy diet rich in antioxidants and omega-3 such as fish, whole grains, and dark leafy greens.
- Exercise regularly.
- Ask your eye doctor if the AREDS2 formula of vitamins and minerals would be beneficial.
- Get regular, dilated eye exams as recommended by your doctor, and use an Amsler grid to monitor your vision.
- Request a referral for a low-vision therapist or occupational therapist in your area. Listen to a conversation with a low-vision specialist about how these professionals can help.
Geographic Atrophy and Mental Health
People living with geographic atrophy often experience emotional hardships including anxiety, feeling powerless, and frustration. Approximately one in three have recently withdrawn from their social lives because of their disease. Learn more about coping with vision loss.
Looking for ways to connect with others?
Join our Community Circle, a monthly, 45-minute program designed to help people with macular degeneration share tips, ask questions, and build community. Meetings are private, held on Zoom, and not recorded. If you are unable to join via Zoom, there is also an option to call in by phone. The meetings are scheduled for the third Friday of each month at 2:00 pm Eastern. Email Amanda Russell at arussell@brightfocus.org to learn more.
The Impact of Geographic Atrophy
In 2022, BrightFocus partnered with Apellis Pharmaceuticals to launch a Harris Poll on a global survey revealing the emotional burden and impact on independence caused by geographic atrophy. It found that:
- Nearly seven in ten geographic atrophy patients believe the impact on their independence and quality of life due to their visual field decline is worse than they expected.
- Most patients feel the disease negatively affects aspects of everyday life like the ability to read, drive, and travel.
- Three out of four patients attributed their vision loss to a natural part of aging before their geographic atrophy diagnosis, reinforcing the opportunity for broad disease education.
Additional Resources
Macular Chats
Free, accessible audio program with leaders in vision research that you can attend by phone or on your computer/streaming device. Visit our webpage to be notified/register for upcoming chats, listen to past programs, or read the transcripts.
Listen to Macular Chats about geographic atrophy:
Download a Brochure
Download a helpful brochure that explains more about geographic atrophy, how it is diagnosed, and questions to ask your eye doctor.
Macular Degeneration Resources
Find out more about macular degeneration and how you can manage care for yourself or a loved one.
AMD Community Circle
Join our monthly Zoom meeting for people with macular degeneration to share tips and ask questions.
Clinical Trials and Other Research Studies
BrightFocus partners with researchers to connect them to people living with Alzheimer’s disease, macular degeneration, geographic atrophy, or glaucoma for other types of research studies such as interviews, focus groups, and surveys.
Clinical Trials: Your Questions Answered
A BrightFocus publication answering all your questions about clinical trials. Read it online or request a printed copy by calling 1-800-437-2423.
Research We Fund
Learn about the innovative scientific research funded by Macular Degeneration Research, a BrightFocus Foundation program.
Resources
Browse Related Resources

Macular Chats
Geographic Atrophy: Making An Informed Treatment Choice
Learn about how to navigate treatment options, engage in shared decision-making with your healthcare team, and maximize your eye health.

Macular Chats
Taking Charge of Your Geographic Atrophy
Hear from guest expert Dr. Veeral Sheth about the latest treatments and research breakthroughs for geographic atrophy, and what you can do to protect your vision.

Podcast
Geographic Atrophy: Your Questions Answered
Guest expert Dr. Philip Niles shared what you need to know about identifying, preventing, and treating geographic atrophy and delved into the landscape of available treatments.

Podcast
Maintaining Emotional Wellness: Living with AMD
Learn about emotional coping strategies and understanding the range of feelings that come with an age-related macular degeneration diagnosis.

Downloadable Resource
Understanding Geographic Atrophy
Some people with age-related macular degeneration (AMD) will develop geographic atrophy, an advanced and severe form of dry AMD that can lead to permanent vision loss. Download a helpful brochure.

Podcast
Treatment Options for Geographic Atrophy
Discover the latest on Geographic Atrophy treatment with Dr. Veeral S. Sheth. Explore advances in dry age-related macular degeneration therapies.


