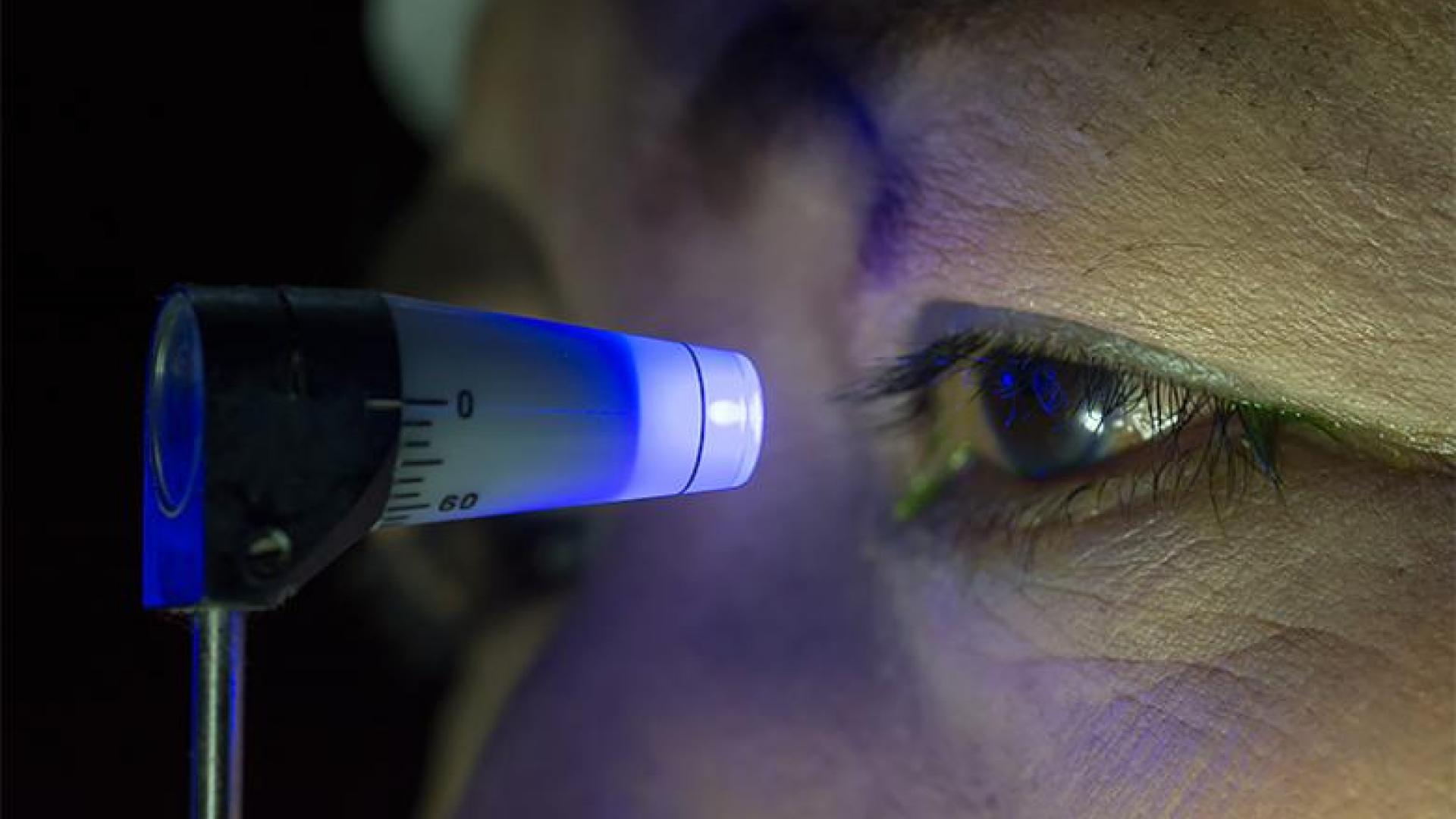
Eye pressure is a very important measurement for ophthalmologists to use when evaluating your eye health. Learn about the various methods of eye pressure measurement (tonometry).
TYPES OF TONOMETRY
- Applanation Tonometry
- Pneumatonometry
- Rebound Tonometry
- Air-Puff Tonometry
- Other Forms of Tonometry
Applanation Tonometry
There are many different ways to measure eye pressure. One such method is a painless procedure, called “applanation tonometry.” The term applanate means to flatten. In most ophthalmologist’s offices, eye pressure is measured using “Goldmann applanation tonometry,” and this is considered a “gold standard” eye pressure measurement.
In this test, the eyes are anesthetized with numbing drops. In addition, a small amount of non-toxic dye is placed in the eye. Your ophthalmologist will instruct you to position your head into a device called the slit lamp. Then, a small tip gently touches the surface of the eye and the eye pressure is measured. The eye pressure is measured based on the force required to gently flatten a fixed area of the cornea.
This test can be affected by various conditions, such as when there is too much or too little dye present in the eye, or depending on the thickness or thinness of the cornea. For example, we know that in thin corneas, which can occur naturally or be induced because a patient has had laser correction eye surgery, the eye pressure measured with this device can be artificially low. In addition, naturally thin corneas are an independent risk factor for glaucoma, so measurement of corneal thickness is part of a comprehensive eye exam and should be performed at your initial and/or subsequent visits.
Pneumatonometry
Alternative measurement methods include pneumatonometry, which is particularly useful in cases of scarred corneas, but can also be used as part of routine practice. In this case, numbing drops are also used but no dye is instilled. The pneumatonometer will also print out a tracing so that the quality of the measurement can be assessed. Pneumatonometry is thought to be less influenced by corneal thickness.
Rebound Tonometry
Rebound tonometry is yet another form of eye pressure measurement. A small plastic-tipped probe bounces gently against the cornea. Numbing drops are not required for this measurement, and there are devices, such as iCare, that can be used at home. It is a portable device and easy to use with children or patients who cannot comply with the more traditional eye pressure measurement techniques. Another device that is portable and easy to use is the Tonopen, a form of electronic indentation tonometry. However, in contrast to iCare, numbing drops are required in order to use the Tonopen.
Air-Puff Tonometry
Non-contact tonometry (or air-puff tonometry) is a form of eye pressure measurement that uses a rapid air pulse to applanate (flatten) the cornea. Although there is some controversy about its accuracy, modern devices have been shown to correlate with Goldmann tonometry.
Other Forms of Tonometry
In addition to the methods of eye pressure measurement mentioned above, there are other forms that you may encounter and also new methods that are being developed. It is important to remember that when you have your eye pressure checked once to 4 or 6 times per year, we are only capturing your eye pressure with a very small “snapshot.” It is known that eye pressure varies over the course of the day, and that these eye pressure fluctuations may be harmful, especially for glaucoma patients. Thus, novel methods have been developed to measure eye pressure over 24 hours, for example, a contact lens that contains an eye pressure sensor (SENSIMED Triggerfish). As of yet these devices are not a part of routine care, but stay tuned for future innovation in this important area of glaucoma care.
About BrightFocus Foundation
BrightFocus Foundation is a premier global nonprofit funder of research to defeat Alzheimer’s, macular degeneration, and glaucoma. Since its inception more than 50 years ago, BrightFocus and its flagship research programs—Alzheimer’s Disease Research, Macular Degeneration Research, and National Glaucoma Research—has awarded more than $330 million in research grants to scientists around the world, catalyzing thousands of scientific breakthroughs, life-enhancing treatments, and diagnostic tools. We also share the latest research findings, expert information, and resources to empower the millions impacted by these devastating diseases. Learn more at brightfocus.org.
Disclaimer: The information provided here is a public service of BrightFocus Foundation and is not intended to constitute medical advice. Please consult your physician for personalized medical, dietary, and/or exercise advice. Any medications or supplements should only be taken under medical supervision. BrightFocus Foundation does not endorse any medical products or therapies.
- Eye Health
- Eye Tests









