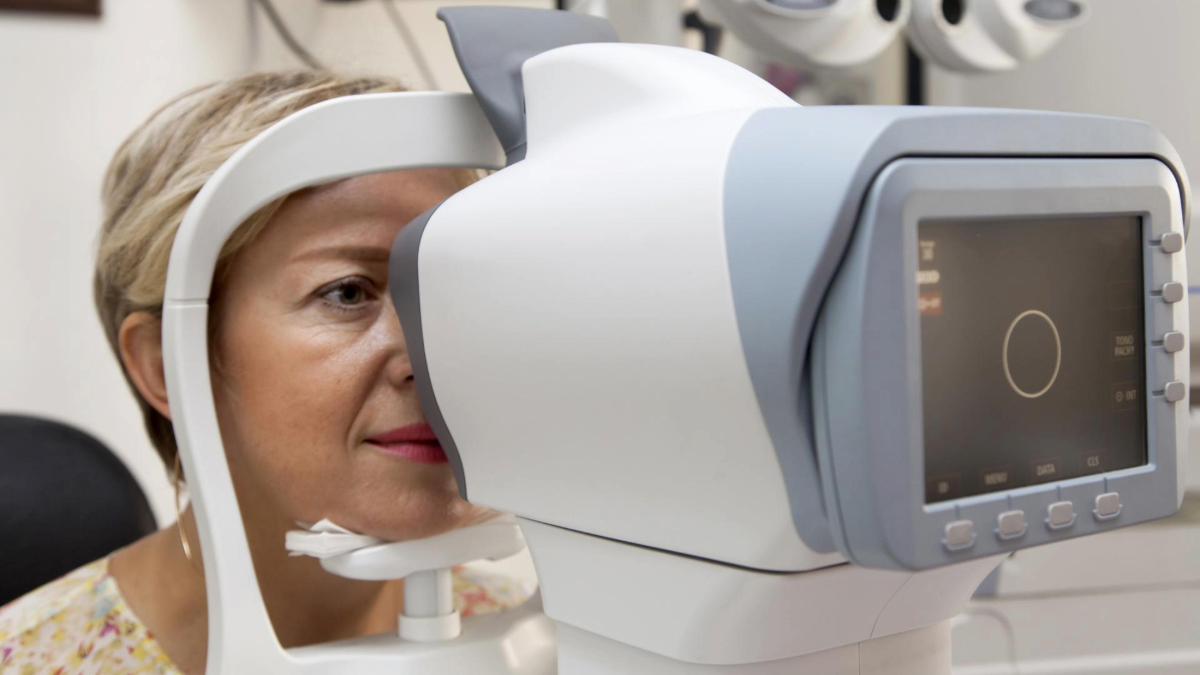
This article summarizes some of the tests that you may experience during an eye exam for glaucoma, including the visual field test, corneal thickness and angle tests, optic nerve imaging, and the eye pressure check.
Glaucoma is an umbrella term, which covers a group of diseases with a characteristic pattern of optic nerve damage. The optic nerve is the bundle of nerve fibers at the back of the eye that carry visual messages from the retina to the brain. There are many types of glaucoma classified by clinical exams. The most common one is primary open-angle glaucoma (POAG). Patients with POAG most commonly experience no symptoms at all until the disease progresses to an advanced stage. The most common symptoms of advanced disease include side vision loss and diminished quality of vision, which can significantly impair daily activities, including driving. The current available treatments have been proven effective in slowing down the disease, but not in reversing optic nerve damage.
In order to avoid such irreversible visual debilitation, it is important to have your eyes examined for glaucoma by an eye doctor, especially if you carry some of the known risk factors, such as family history of the disease. It is crucial to have some basic understanding of the tests for glaucoma so that you can make an informed decision about your treatment options under the guidance of your doctor. Some of the tests are outlined below.
Eye Pressure Check
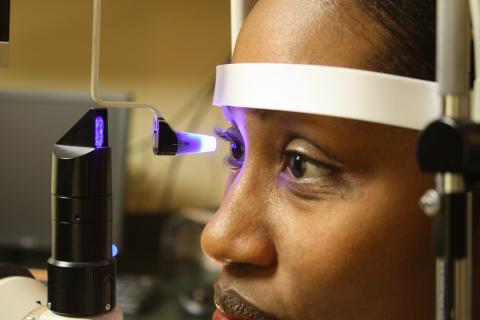
An eye pressure test, called tonometry, is the most common method of checking for increased eye pressure.
Visual Field Test
A visual field test is considered a functional test, and allows your doctor to tell you if you have lost any field of vision from glaucoma, how much you have lost, and can help determine the rate of disease progression, which in turn will help to tailor the treatment. Your doctor will be able to tell you how severe your disease is based on this test.
Although the test is not painful, and it only takes a few minutes for each eye, if you are overly anxious or tired, you may not be able to perform the test reliably. Also, the test may require some learning experience, and therefore may need to be repeated. There is no special preparation for the test, or any need to remove your contact lenses. The visual field test needs to be repeated periodically, although the frequency may vary significantly depending upon your specific situation.
Watch: Glaucoma Testing
Glaucoma Imaging Tests
Glaucoma imaging tests are a reliable way for your doctor to monitor glaucoma progression. The tests are non-invasive and involve no radiation. Your pupils will be dilated using eye drops, and then the doctor will photograph your optic nerve with a digital camera or use other technologies (optical coherence tomography) to map your optic nerve. Regardless of the modality your doctor chooses, the results become immediately available, which can be projected on a computer screen for discussion.
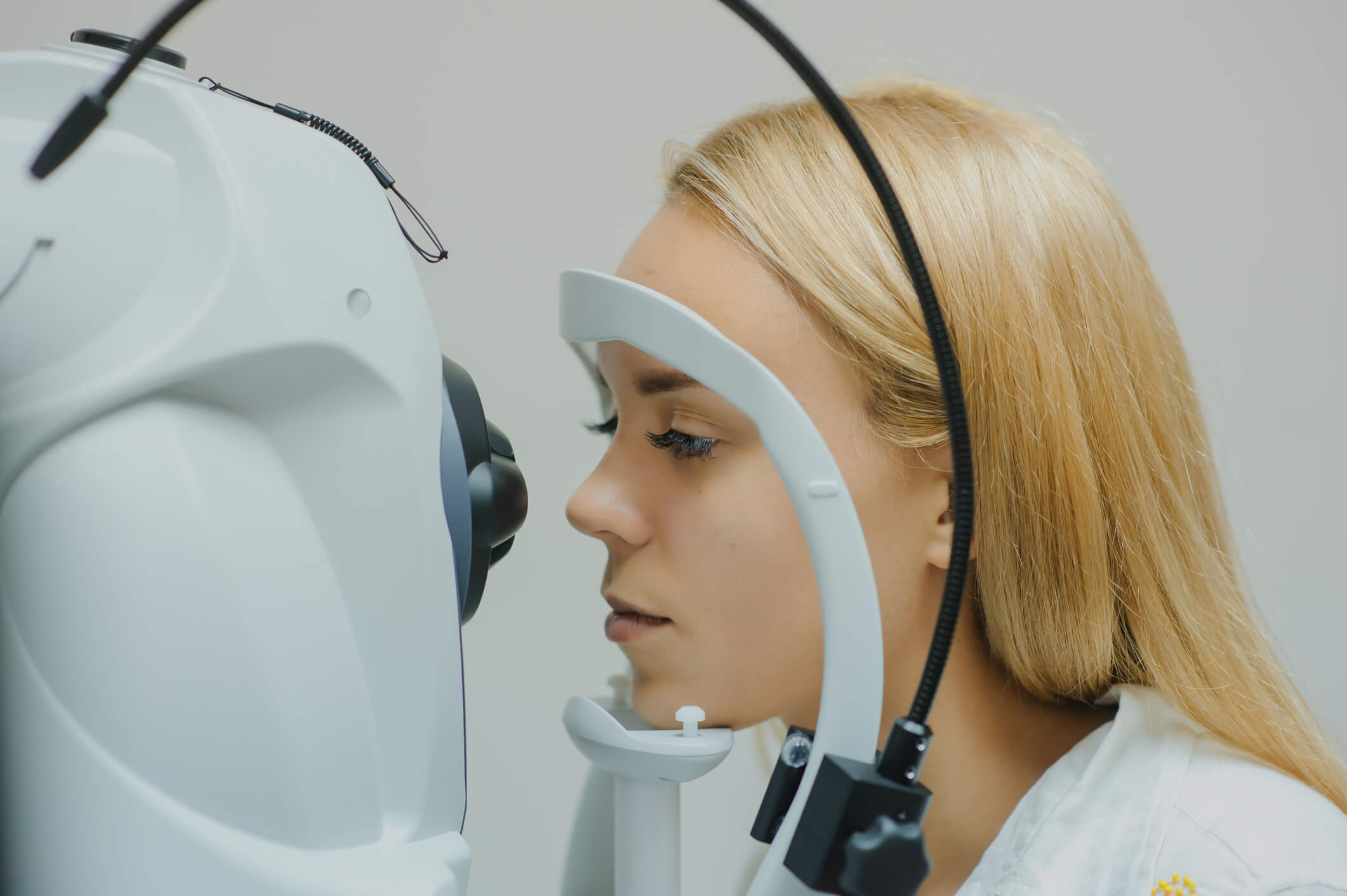
The Dilated Eye Exam
A comprehensive evaluation will also include a dilated eye exam. In assessing your glaucoma, the ophthalmologist will dilate your eyes so that he or she can get a magnified, 3D view of your optic nerve. This helps to determine the status of your optic nerves and glaucoma. He or she will assess the shape, color, depth, size, and vessels of the optic nerve. In addition, an examination of the central and peripheral retina will be performed.
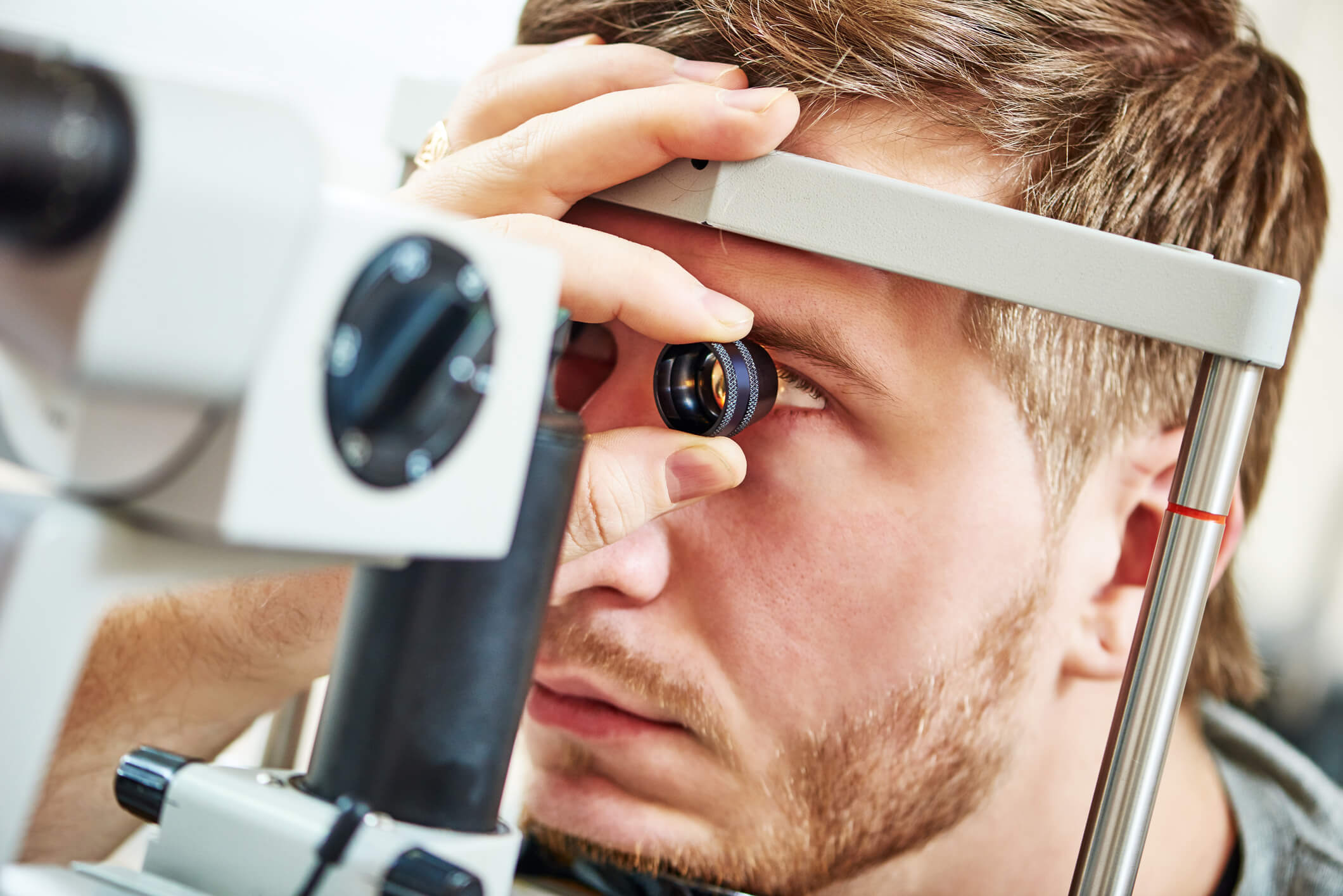
Corneal Thickness and “Angle” Tests
Some other contact tests include a corneal thickness test (pachymetry) and an “angle” test (gonioscopy). They are absolutely necessary and are included in the “vital signs” of the eye exam.
Cornea Thickness Test (Pachymetry)
Pachymetry painlessly measures the thickness of the cornea with a small probe after the eye is numbed with an eye drop. A thin cornea may contribute to artificially low eye pressure readings, and a thick cornea may contribute to pressure readings that are higher than they actually are. It is also known that thin corneas are a risk factor for glaucoma. The cornea thickness measurement provides crucial information for your doctor to tailor your treatment.
Angle Test (Gonioscopy)
Gonioscopy is another test performed by your doctor with a hand held goniolens. Some doctors refer to the lens as an “exam contact lens.” The doctor will barely touch the gonioscopy lens to the numbed cornea. The procedure is simple, quick, and does not hurt. It is similar to using mirrors in a periscope to see areas that are not otherwise visible to the naked eye. Once the gonioscopy lens is in contact with the cornea, it will allow the eye doctor to see the “angle.” The “angle” is the area where the cornea (the clear part in the front of the eye) meets the iris (the colored part of the eye). The “angle” is also where the trabecular meshwork is located. Under normal circumstances, the majority of the fluid that is created inside the eye must exit the eye by passing through the trabecular meshwork. If the trabecular meshwork is visible on gonioscopic examination, doctors call this an “open” angle. If the trabecular meshwork is blocked by scar tissue or the iris, it is called a “closed” angle.
Summary
We have discussed some of the important components of your eye exam for glaucoma. There are some special tests that are unique to glaucoma diagnosis and monitoring of the disease. If you have any questions about the tests or results, ask your ophthalmologist to discuss these issues with you.
Six Common Glaucoma Tests
- Eye Pressure Check
The eye pressure test is called tonometry, and the most common method is known as “applanation,” in which a tiny instrument contacts the surface of the eye after it is numbed with an eye drop. - Visual Field Test
The visual field test allows your doctor to tell you if you have lost part of your field of vision from glaucoma, how much you have lost, and can help determine the rate of disease progression, which in turn will help to tailor the treatment. - Glaucoma Imaging Tests
Your pupils will be dilated using eye drops, and then the doctor will photograph your optic nerve with a digital camera, or use other technologies (OCT) to map and document the health of your optic nerve. - The Dilated Eye Exam
In assessing your glaucoma, the ophthalmologist will dilate your eyes so that he or she can get a magnified, 3D view of your optic nerve. This helps to determine the status of your optic nerves and glaucoma. - Cornea Thickness Test (Pachymetry)
Pachymetry painlessly measures the thickness of the cornea with a small probe after the eye is numbed with an eye drop. Corneal thickness can affect eye pressure readings. - Angle Test (Gonioscopy)
This test allows the eye doctor to see the “angle,” where the cornea (the clear part in the front of the eye) meets the iris (the colored part of the eye). The “angle” is also where the trabecular meshwork (the eye’s drainage system) is located.
About BrightFocus Foundation
BrightFocus Foundation is a premier global nonprofit funder of research to defeat Alzheimer’s, macular degeneration, and glaucoma. Since its inception more than 50 years ago, BrightFocus and its flagship research programs—Alzheimer’s Disease Research, Macular Degeneration Research, and National Glaucoma Research—has awarded more than $300 million in research grants to scientists around the world, catalyzing thousands of scientific breakthroughs, life-enhancing treatments, and diagnostic tools. We also share the latest research findings, expert information, and resources to empower the millions impacted by these devastating diseases. Learn more at brightfocus.org.
Disclaimer: The information provided here is a public service of BrightFocus Foundation and is not intended to constitute medical advice. Please consult your physician for personalized medical, dietary, and/or exercise advice. Any medications or supplements should only be taken under medical supervision. BrightFocus Foundation does not endorse any medical products or therapies.
- Eye Tests









