Sometimes it can be difficult to see an item you’re looking for amongst the clutter in your house. Most people have misplaced their keys only to overlook them several times because the keys aren’t in their usual spot.
A degenerative vision disorder takes that a step further. What if your brain cannot process all the items you see, and that is why you can’t see your keys sitting among the clutter?
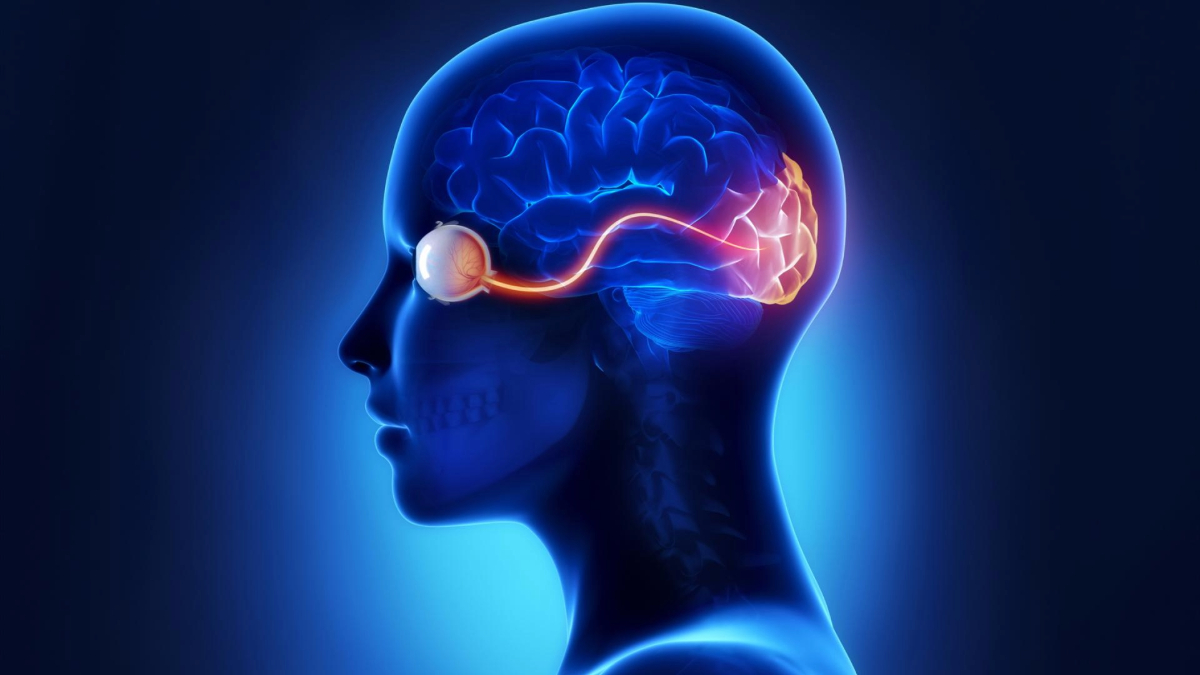
Images captured by the eye are processed in the visual center at the back of the brain. When the brain suffers progressive damage to its vision center, it can keep a person from seeing the whole picture.
Read on to learn more about posterior cortical atrophy, an atypical form of Alzheimer’s that starts with visual disturbances.
What is Posterior Cortical Atrophy?
Posterior Cortical Atrophy (PCA), also known as Benson syndrome, is an atypical degenerative disease that damages the visual center of the brain.
Symptoms of Posterior Cortical Atrophy
People with PCA may experience difficulties with:
- Daily tasks (e.g. getting dressed)
- Reading
- Drawing
- Puzzles
- Understanding where objects are in space
- Driving/ judging distances
- Seeing the whole picture in front of them
- Calculations
A unique disease feature is a person’s inability to see everything in a picture. At home, this can make clutter especially difficult to work around. Someone living with PCA may not see that a chair is in their walking path and swerve to avoid it, or not see the milk in the fridge when the carton is right in front of them.
Is it Alzheimer’s?
PCA is considered an atypical, non-memory form of Alzheimer’s that is present in roughly 1 in 10 affected people. It’s most commonly found in those with sporadic young-onset Alzheimer’s, which impacts people under 65 years old who do not carry a dominant family gene for the disease. However, PCA is also associated with other kinds of dementia and neurological conditions, like dementia with Lewy bodies.
For PCA due to Alzheimer’s, researchers believe that hallmark disease proteins amyloid-beta (Aβ) and tau, often found in the brain’s learning center, instead appear in the visual center. Vision is normally the last area to show any biological signs of Alzheimer’s, suggesting that the disease proteins have changed their typical distribution throughout the brain. Now these abnormal proteins affect the areas that harbor the most basic visual information, like seeing dots and lines and associating them with one another. Research is ongoing to determine possible underlying causes that may direct disease proteins to target the visual picture in these cases.
Diagnosis
Often, a person will see their eye doctor first to complain of problems with reading or other activities—thinking that their glasses aren’t working any longer. A person with PCA may also show secondary signs, such as significant behavioral changes, including anxiety, irritability, depression, and apathy.
A doctor will perform a comprehensive examination to rule out eye diseases but may begin to suspect a brain disease and refer to a neurologist. There is no singular test for PCA; a doctor will need to perform a full examination of the eyes and brain to render a diagnosis. First, a neurologist will need to determine what core features of PCA are present and whether these issues have appeared over time and progressively worsened. They will also rule out other possible causes for the symptoms, like a tumor. Some people may not find a clear answer; but through increased education and partnership with eye doctors, more people living with PCA are finding the care they need.
Biology can help guide the way to identify the presence of a neurodegenerative disease like Alzheimer’s. A neurologist may use specialized brain scans or look at fluid biological markers to confirm their proposed diagnosis. For example, if the doctor suspects Alzheimer’s disease to underlie the symptoms, they can look at the levels of Aβ and tau protein in the blood or cerebrospinal fluid, or they can run a targeted PET scan. This helps better inform and finalize the diagnosis and in preparing a treatment plan.
This approach to diagnosing PCA was applied in a large international study conducted in 2024. Data from 36 research centers studying PCA found that many participants showed Alzheimer’s indicators in their biological workup, confirming the suspected diagnosis. The team also found that Alzheimer’s disease was the most common underlying neuropathology (brain disease) at autopsy.
Treatment
There are no approved treatments specific to PCA, though some interventional strategies may make the condition more manageable. Medications and therapies are available to assist with mental health challenges and to better preserve daily life skills potentially impacted by PCA. Further, caregivers can also take steps to make the home more accessible for their loved one, like carefully arranging furniture to provide clear walkways and minimize accidents. Minimizing clutter, removing throw rugs/ opting for non-skid floor coverings, and labeling drawers can also help to make the home a safer place.
Someone with PCA due to Alzheimer’s may opt to use treatments approved for Alzheimer’s disease. However, studies are underway to see if they will improve PCA symptoms. Those with PCA are also at higher risk for a condition called cerebral amyloid angiopathy, in which amyloid protein builds up in brain blood vessels. This may impact their eligibility to take amyloid-targeting therapies approved for Alzheimer’s disease because of a rare side effect called amyloid-related imaging abnormalities (ARIA). More research is needed to determine if PCA patients receiving anti-amyloid therapies are at higher risk for ARIA.
Summary
Atypical forms of Alzheimer’s, like PCA, are getting more research attention now than ever. Improved diagnostic criteria and collaboration between healthcare providers has catalyzed better care for those living with this condition. While there is no cure for PCA, resources are available for caregivers and their loved ones to create more accessible living conditions and preserve quality of life for those affected by this disease. To find more Alzheimer’s disease resources, visit our page.
About BrightFocus Foundation
BrightFocus Foundation is a premier global nonprofit funder of research to defeat Alzheimer’s, macular degeneration, and glaucoma. Since its inception more than 50 years ago, BrightFocus and its flagship research programs—Alzheimer’s Disease Research, Macular Degeneration Research, and National Glaucoma Research—has awarded more than $330 million in research grants to scientists around the world, catalyzing thousands of scientific breakthroughs, life-enhancing treatments, and diagnostic tools. We also share the latest research findings, expert information, and resources to empower the millions impacted by these devastating diseases. Learn more at brightfocus.org.
Disclaimer: The information provided here is a public service of BrightFocus Foundation and is not intended to constitute medical advice. Please consult your physician for personalized medical, dietary, and/or exercise advice. Any medications or supplements should only be taken under medical supervision. BrightFocus Foundation does not endorse any medical products or therapies.
- Disease Biology








