Our Approach to Macular Degeneration Research
Macular Degeneration Research, a BrightFocus Foundation program, takes a 360-degree approach to fund innovative scientific research worldwide to defeat macular degeneration, exploring the full range of scientific paths toward better treatments and ultimately a cure. From exploring ways to regenerate damaged cells to the influence of early-life events, diet, and nutrition on disease risk, we leave no stone unturned in the quest for a cure.
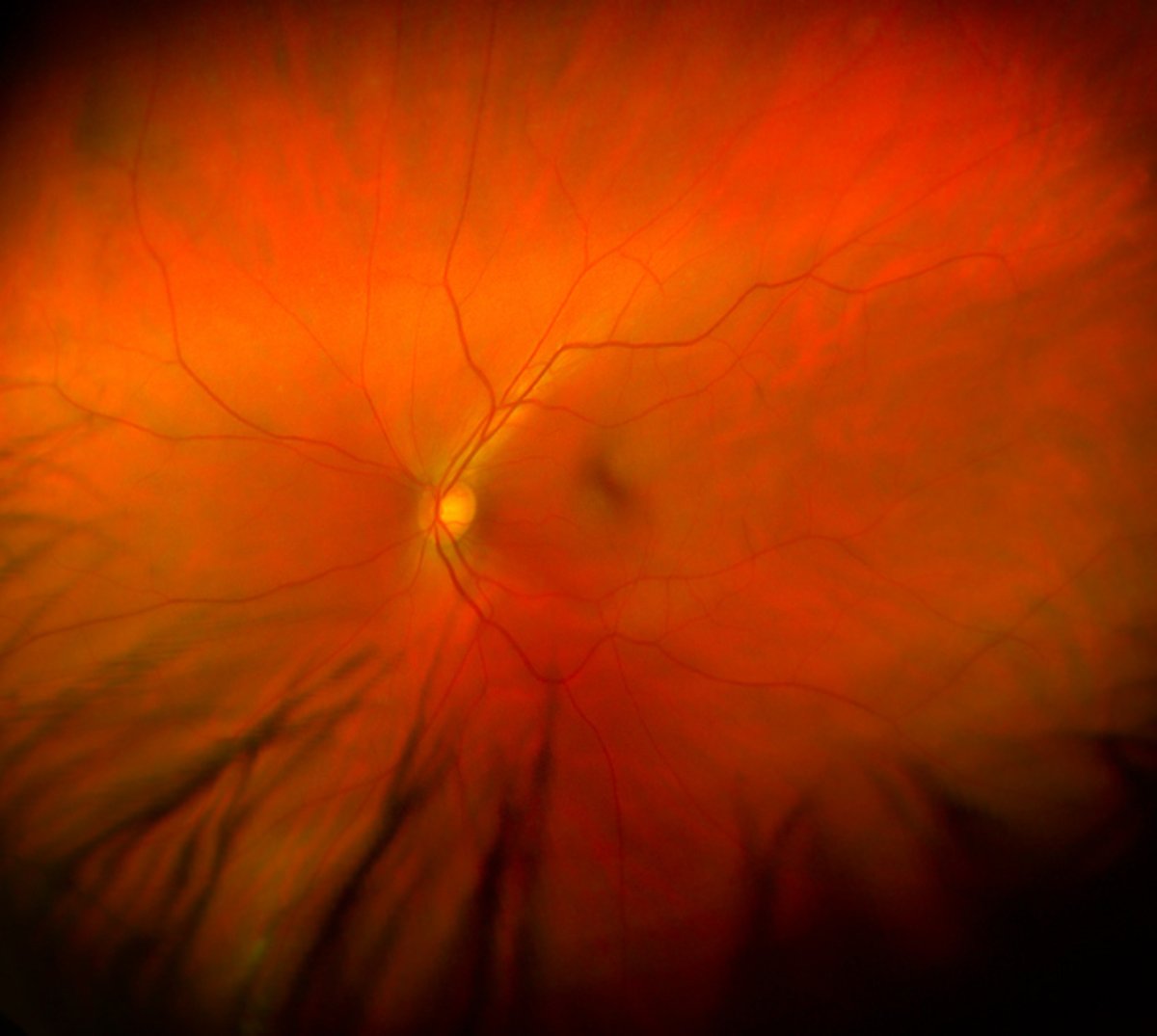
Cell Metabolism
The retinal pigment epithelium (RPE) is a single layer of cells at the back of the eye next to the retina. Its health and ability to support the nerve cells of the retina depend on well-functioning cell metabolism as a source of energy.
Macular Degeneration Research grantees are investigating the decline in cellular energy production in the RPE and the mitochondria, which are the cell’s “powerhouse” for energy production, as possible triggers of age-related macular degeneration. They are also exploring how an imbalance between energy needs and production could contribute to the disease and are finding ways to restore health to the aging eye by improving cellular metabolism.
Diet & Nutrition’s Impact
Our diets help shape a healthy immune response, including through effects on the microorganisms that live on and inside our body, such as gut bacteria. The current treatment for preventing the progression of intermediate age-related macular degeneration is a supplement combination that showed effectiveness in two large National Institutes of Health studies.
The AREDS2 (Age-Related Eye Disease Study 2) eye formula combines vitamins C and E, the pigments lutein and zeaxanthin, and zinc and copper. Investigators are exploring how to increase uptake of carotenoids (pigments like lutein and zeaxanthin that give fresh produce their bright red, yellow, and orange colors), an important nutrient in macular health. A Mediterranean-style diet rich in fish, whole grains, fruits, and leafy vegetables also is of interest.
Research shows there may be additional ways to lower risk, given how sensitive the eye is to nutritional intake and possible deficiencies. Ideally, these dietary findings will translate into clinical use and “vision-healthy” lifestyles.
Drusen Formation & Immune Response
As the eye ages, it becomes less efficient at removing waste. Deposits of extracellular waste products containing fats and proteins, known as drusen, may collect within and beneath the retinal pigment epithelium cell layer and trigger an immune response. In fact, when spotted on a comprehensive eye exam, drusen often are the first sign of age-related macular degeneration, or AMD; increases in the number and size of drusen may cause the immune system to kick into overdrive.
Ultimately, an out-of-control immune response may reach a tipping point and damage cells in the macula, or central part of the eye, which provides sharp central vision. Researchers are therefore focusing on specific aspects of the immune response, including testing drugs that can clear the waste deposits that contribute to AMD.
Genes & Age-Related Macular Degeneration
Most forms of macular degeneration are not linked to any single genetic mutation. Instead, susceptibility to age-related macular degeneration, or AMD, is scattered over a number of small irregularities of genes called single nucleotide polymorphisms (SNPs). SNPs can arise spontaneously or be inherited, and their impact is tempered by factors such as age, overall health and nutrition, and exposure to cigarette smoke, sunlight, and other toxins. Targeted gene research could lower the risk of AMD by blocking or replacing signals from genes that trigger disease and defend retinal pigment epithelium cells against oxidative stress from aging and other causes.
Geographic Atrophy
Some people with age-related macular degeneration, or AMD, will develop geographic atrophy, an advanced and severe form of dry age-related macular degeneration that can lead to permanent vision loss. In geographic atrophy, regions of cells in the retina waste away and die (atrophy), resulting in dead zones and an expanding blind spot near the center of the visual field.
The first treatments for geographic atrophy were approved by the Food and Drug Administration in 2023, and several other promising treatments are undergoing testing in clinical trials. Macular Degeneration Research is funding innovative research into new drugs and ways to manage and treat this complex form of AMD responsible for around 20% of cases of legal blindness in North America.
Innovative Approaches to Treatments
One day, we may be able to detect signs that age-related macular degeneration, or AMD, is developing and take early steps to defend against it. Macular Degeneration Research is funding research into unique ways to protect the retinal pigment epithelium and retina before sight damage has occurred, including drugs that enhance immune functioning and improve the eye’s ability to clear lipids/fats and other waste that could lead to inflammation in AMD. New imaging techniques will support better tracking of disease progression over time, and gene therapy is being evaluated as a possibility for treating AMD.
Regenerating Damaged Cells
Unlike human skin, the nerve cells of the eyes do not typically regrow or regenerate after damage has occurred. But there is new hope for overcoming this biological limitation. Work is moving forward to regenerate and reconnect the eye’s retinal cells that have been damaged by age-related macular degeneration, or AMD, and to restore the underlying retinal pigment epithelium (RPE) cells. Grantees are recreating parts of the eye using human-induced pluripotent stem cell (iPSC) technology—stem cells created from living adult tissue. Cell regeneration in animal models also is being studied for its applicability to human therapy.
News
Explore Our Research

Article
Shaping the Future of Macular Degeneration Research: Key Takeaways from the 2025 AMD Fast Track Workshop
BrightFocus Foundation’s 2025 Age-Related Macular Degeneration (AMD) Fast Track brought together early-career and established scientists to accelerate research toward a cure for AMD.
Article
How Understanding Lipid Processing in the Eye Could Spark Innovative AMD Treatment Approaches
With the help of funding from Macular Degeneration Research, Dr. Neetu Kushwah is studying the link between abnormal lipid regulation in the eye, inflammation, and age-related macular degeneration. Her findings could inspire new methods for treating the disease.

Article
Early Research Funding Is Essential to Saving Sight From Macular Degeneration
Medicine's biggest breakthroughs often start out as the smallest of ideas. BrightFocus Foundation’s Macular Degeneration Research supports bold, early-stage science across a wide range of approaches.

Article
New Supplement to Prevent Macular Degeneration Inspires Deeper Search for Cures
A Macular Degeneration Research-funded scientist launched a supplement based on a link he discovered between the eye disease and Parkinson’s disease. Now he’s continuing research in the hopes of finding novel cures.

Article
Transforming Macular Degeneration Care With Long-Acting Treatment
With funding from Macular Degeneration Research, Dr. Daisy Shu is exploring advanced drug delivery systems that release medicine slowly over time. This innovative approach could reduce the number of injections needed for macular degeneration while maintaining vision-saving results.
Article
How Targeting a Molecular 'Switch' Could Inspire New Macular Degeneration Treatments
A researcher funded by BrightFocus’ Macular Degeneration Research is zeroing in on a protein that damages eye cells in the early stages of dry age-related macular degeneration, offering insights that could lead to new treatments.

Article
How Better Models of Macular Degeneration Could Help Prevent Vision Loss
Most experimental models that researchers use to study macular degeneration fall short. BrightFocus Macular Degeneration Research grant recipient Dr. Brittany Carr aims to change that.
Article
Is This the Next Best Thing to Regrowing a New Retina?
A BrightFocus Macular Degeneration Research-funded scientist is investigating a new regeneration technique to restore key cells that are wiped out in late-stage age-related macular degeneration.
Article
Turning Back the Biological Clock on Aged and Injured Eye Cells
A de-aging technique offers hope for halting damage in early macular degeneration.


