
Learn about the causes, symptoms, treatment, and prevention of neovascular glaucoma.
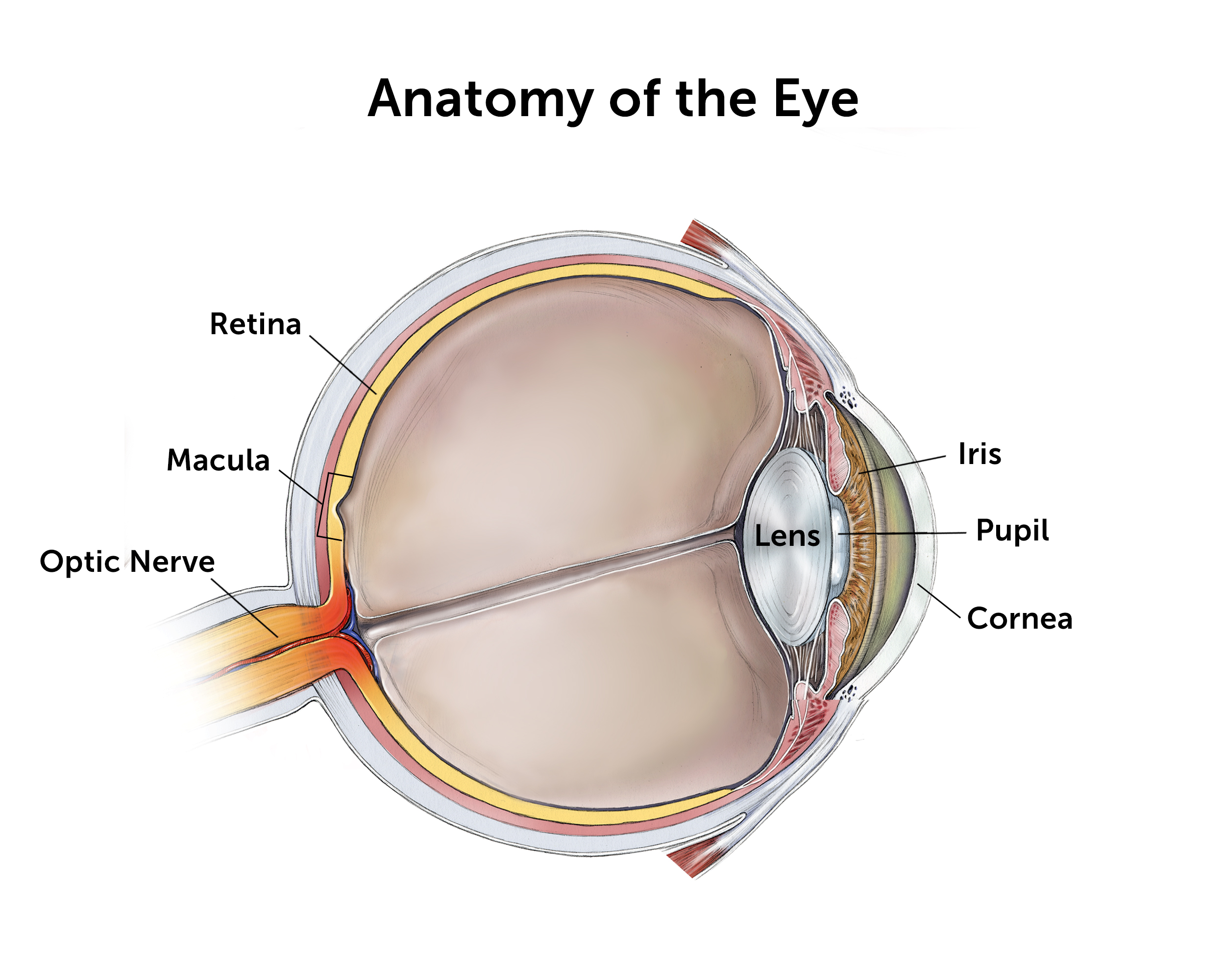
Neovascular glaucoma is a type of secondary glaucoma where the angle of the eye is closed by “new blood vessels,” hence the name “neovascular.” The “angle” referred to here is the angle between the iris, which makes up the colored part of your eye, and the cornea, which is the clear-window front part of your eye.
Neovascular glaucoma typically develops in eyes in which there is severe retinal vein blockage or severe diabetic eye disease. There are other causes too, including chronic retinal detachment, tumors, and ocular ischemic syndrome, although these are all much rarer causes and will not be discussed in this article.
Abnormal Blood Vessel Growth
In healthy eyes, the iris and drainage angle where the trabecular meshwork lies typically do not have abnormal vessels growing on them. The trabecular meshwork is the spongy tissue located near the cornea through which eye fluid (aqueous humor) flows out of the eye. In neovascular glaucoma, the new vessels form in these areas, and often they are leaky or cause inflammation.
New blood vessels growing over the drainage angle can cause scarring and narrowing, which can eventually lead to complete closure of the angle. This process results in elevated eye pressure since the fluid in the eye cannot access the drainage system. In cases of neovascular glaucoma, the eye is often red and painful, and the vision is abnormal.
Watch: Where is Eye Fluid Produced?
Causes of New Blood Vessel Growth
In the case of a retinal vein blockage or diabetic eye disease in the retina, the retina becomes “ischemic,” meaning it does not have enough oxygen flowing to it. The retina begins to release chemicals to counteract the ischemia, including vascular endothelial growth factor (VEGF).
VEGF leads to new blood vessel formation, which theoretically could bring more oxygen to the sick “ischemic” retina. However, in the case of these diseased retinas, the new blood vessels are leaky and abnormal. For example, in patients with diabetic retinopathy, there is bleeding of these abnormal vessels. Sometimes the bleeding can be so severe that the back of the eye, the vitreous cavity, fills with blood (vitreous hemorrhage). The VEGF being released by the ischemic retina also migrates to the front of the eye, where it causes new blood vessel formation on the iris and in the drainage angle.
Symptoms
The symptoms of a retinal vein blockage or diabetic retinopathy can include vision loss, although sometimes patients can still have good vision. These retinal diseases are often diagnosed because the patient experiences vision loss and seeks care, or they are diagnosed during a routine annual examination. Diabetic patients should have yearly dilated examinations to evaluate for diabetic retinopathy, and more often if they have mild forms of diabetic retinopathy.
The symptoms of neovascular glaucoma can include pain, redness, and decreased vision, although in early stages of the disease it is possible not to have any symptoms.
Treatment
Treatment of neovascular glaucoma includes two parts:
- Treat the underlying cause of neovascular glaucoma, that is, the ischemic retina; and
- Lower the eye pressure, whether through medications, laser, surgery, or a combination of these types of treatments.
Treatment of the ischemic retina includes using a retinal laser (pan-retinal photocoagulation), which decreases the retina’s production of VEGF, and injections of anti-VEGF medications into the eye, which will cause the abnormal blood vessels to start regressing or disappearing.
It is extremely important to treat the underlying cause of neovascular glaucoma, so often your care may include several specialists, such as a glaucoma and retina specialist. It is also possible that you will be treated by a comprehensive ophthalmologist. Your primary care doctor should also be included as part of the team, as will be discussed below in the prevention section.
If glaucoma drops fail to bring the pressure down adequately, surgery is often the next step. In neovascular glaucoma, there are many considerations for what surgery to choose, including the potential of recoverable vision. Tube shunt surgery is the usual surgery recommended for patients, as it can bring down the pressure immediately and has higher rates of success than other filtering surgeries, such as trabeculectomy. If vision is very poor, some ophthalmologists may recommend a less invasive procedure such as a type of laser that destroys the ciliary body, the part of the eye that produces fluid.
Prevention
Prevention should be focused on preventing the most common underlying causes of neovascular glaucoma, including retinal vein blockage and diabetic retinopathy. Risk factors for these retinal diseases include age, high blood pressure, diabetes, and heart disease. Indeed, for some types of vein occlusion, high eye pressure is a risk factor.
Controlling blood pressure and diabetes is extremely important, and patients and their ophthalmologists should work with the primary care team to ensure these goals are met. For diabetics especially, another key prevention measure is a yearly dilated exam, and for all individuals ages 65 years and older, a comprehensive eye exam every 1 to 2 years is recommended. The American Academy of Ophthalmology also recommends a baseline comprehensive eye examination at age 40.
About BrightFocus Foundation
BrightFocus Foundation is a premier global nonprofit funder of research to defeat Alzheimer’s, macular degeneration, and glaucoma. Since its inception more than 50 years ago, BrightFocus and its flagship research programs—Alzheimer’s Disease Research, Macular Degeneration Research, and National Glaucoma Research—has awarded more than $330 million in research grants to scientists around the world, catalyzing thousands of scientific breakthroughs, life-enhancing treatments, and diagnostic tools. We also share the latest research findings, expert information, and resources to empower the millions impacted by these devastating diseases. Learn more at brightfocus.org.
Disclaimer: The information provided here is a public service of BrightFocus Foundation and is not intended to constitute medical advice. Please consult your physician for personalized medical, dietary, and/or exercise advice. Any medications or supplements should only be taken under medical supervision. BrightFocus Foundation does not endorse any medical products or therapies.
- Eye Health









